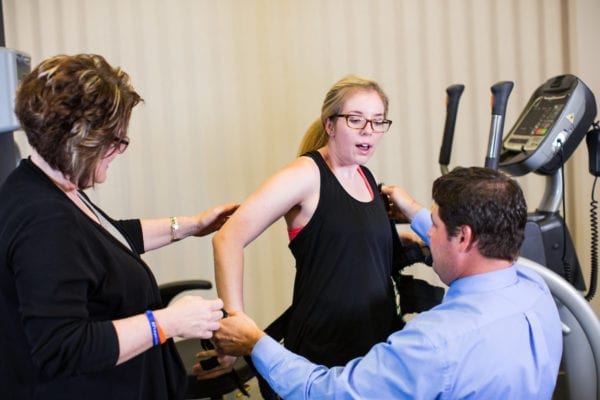
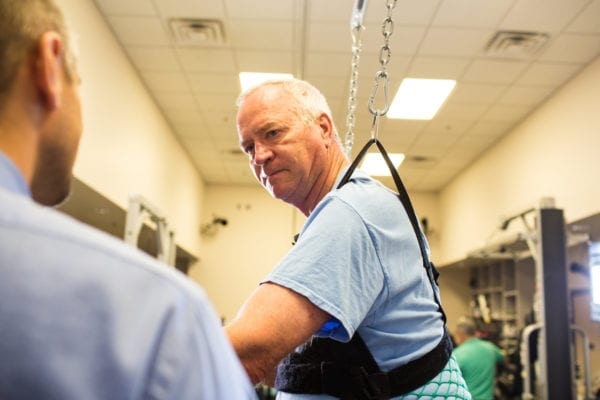
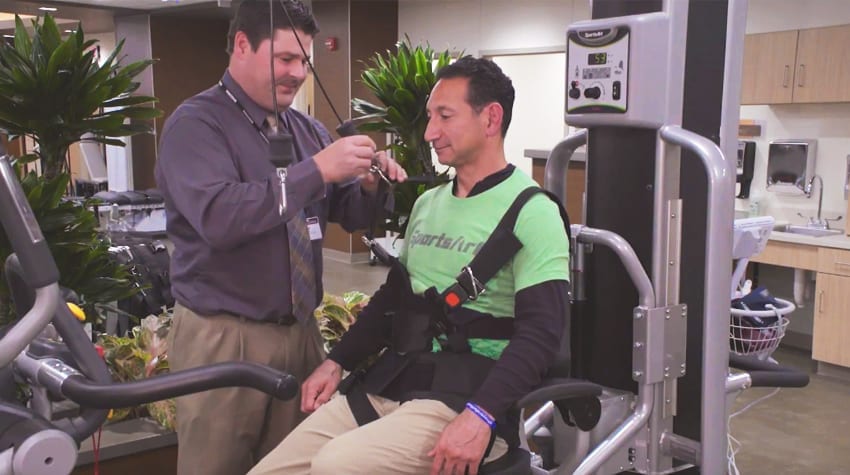
EMPOWERING PATIENTS, ASSISTING CLINICIANS
ICARE’s intelligent control provides a movement that is neither always assistive nor always resistive. It is designed to provide an
“assist as needed” approach similar to what a therapist provides physically and intuitively while gait training a patient. The ICARE frees clinicians
from hours of strenuous manual lifting and improves patient access to assistive technology, allowing them to improve their walking and fitness.
Relearning to walk and remaining physically active are important rehabilitation goals for individuals with weakness, numbness or balance problems and those recovering from a disabling injury or illness. To regain walking ability, thousands of step-like movements are required to achieve lasting neuroplasticity gains. Often these individuals face barriers due to the lack of equipment that appropriately accommodates the needs of compromised muscles. Enter ICARE.
Developed at the Madonna Rehabilitation Hospital and Research Institute in Lincoln, Nebraska, ICARE is a fully-integrated system that provides a safe, effective method for assisting patients with neuromuscular disorders resulting from stroke, TBI, partial SCI, and other injuries or diseases. ICARE’s intelligent control provides a movement that is neither always assistive or always resistive. It is designed to provide an “assist as needed” approach that is similar to what a therapist provides physically and intuitively while gait training a patient. The ICARE frees clinicians from hours of strenuous manual lifting and advancing of the legs and expands patient access to assistive technology, allowing them to improve their walking and cardiovascular fitness.
ICARE’s leg movements closely mimic the kinematic and electromyographic (EMG) patterns of walking. Noted in development studies, ICARE training can help individuals regain or retain the flexibility and strength required for walking, particularly if the muscle demands are customised to those with weakness during rehab. Special focus was applied during development to ensure the appropriate levels of assistance are available for individuals to accomplish the required repetitions, both with partial body weight support and motor-assistance from the footplates.


COMPLETE ICARE SYSTEM
ICARE ELLIPTICAL
-
Movement patterns emulate motion and muscle demands of walking
-
Forward and reverse motor assistance allows speeds up to 65 cycles
per minute -
Adaptive motor assistance automatically adjusts to suit patient’s
exercise needs -
Adjustable stride range from 18–29 in. with fingertip shift-on-the-fly controls
-
Arms can be integrated into training for complete body workout
-
Contact and telemetry heart rate monitoring
-
Remote control for easy, unobtrusive clinician adjustments
-
Passcode control of motor-assisted features allows use of non-motor
assisted training features by others -
Infrared safety system shutdown reduces risk of injury
WHEELCHAIR RAMP, STAIRS AND CLINICIAN PLATFORM
-
Provides access for clients who use a wheelchair and eases transfers
on/off the device -
Raises clinician’s viewing position for unobstructed monitoring
BODY UNWEIGHTING SYSTEM
-
Electronically controlled pneumatic height-adjustable seat provides 90° rotation in either direction and arm rests flip up for easy patient access
-
Unweighting harness supports and lifts up to 400 lbs of patients’ body weight

ICARE PLUS SYSTEM

Includes all features listed for ICARE Elliptical and body unweighting system
ICARE MOTOR-ASSISTED SYSTEM

Includes all features listed for ICARE Elliptical
| FACILITY | LOCATION |
|---|---|
| Individual Home User | Berkley, CA |
| Rancho Los Amigos National Rehab Center | Downey, CA |
| Casa Colina Hospital | Pomona, CA |
| VA Medical Center, Vs #135 | Washington, DC |
| CORE Center of Recovery and Exercise | Altamonte Springs, FL |
| Mercy Hospital | Coconut Grove, FL |
| Rehabilitation Institute of Northwest Florida | Destin, FL |
| Lawnwood Regional Medical Center | Fort Pierce, FL |
| Brooks Rehabilitation Hosp | Jacksonville, FL |
| NextStep Orlando Project Walk Orlando | Longwood, FL |
| Orange Park Medical Center | Orange Park, FL |
| Osceola Regional Medical Center | Orlando, FL |
| UCF Lake Nona Hospital | Orlando,FL |
| Romain Rehabilitation Center | Pembroke Pines, FL |
| West Florida Hospital | Pensacola, FL |
| Redmond Regional Medical Center | Rome, GA |
| Eastside Medical Center | Snellville, GA |
| Unity Point Health Younker Rehabilitation Clinic | W Des Moines, IA |
| Exercisabilities Brennan | Rochester, MN |
| Cameron Regional Medical Center | Cameron, MO |
| Ability KC | Kansas City, MO |
| Madonna Proactive | Lincoln, NE |
| Madonna Rehab Hospital | Lincoln, NE |
| QLI Quality Life Inc. | Omaha, NE |
| Individual Home User | Orleans, NE |
| Optimal Physical Therapy- Lake Mead | Las Vegas, NV |
| Individual Home User With SCI | Altamont, NY |
| Good Shepherd Rehab Hospital | Allentown, PA |
| Individual Home User | Doylestown, PA |
| The Montreal Neurofeedback Center | Montreal, QC |
| Parkridge Medical Center | Chattanooga, TN |
| HCA Hospital Corporation Of America | Nashville, TN |
| Individual Home User | Huffman, TX |
| Individual Home User | Laredo, TX |
| Medical Center Of Plano | Plano, TX |
| Lewis Gale Hospital | Salem, VA |
| Simply Movement | Victoria, Australia |
| Quimcolor Ltda | Santiago De Chile, Chile |
| Neuro Trauma Center/Alex Andres Coello Diaz | Bucaramanga, Colombia |
| Ortokids Internacional | Chorrillos, Peru |
Up to November 2020
SELECTED ARTICLES AND BOOK CHAPTERS
- Fallahtafti F, Pfeifer CM, Buster TW, Burnfield JM (2020). Effect of motor-assisted elliptical training speed and body weight support on center of pressure movement variability. Gait and Posture, 81: 138-143. DOI: 10.1016/j.gaitpost.2020.07.018.
- Burnfield JM, Cesar GM, Buster TW (2020). Variations in plantar pressure variables across elliptical trainers in older adults. Available online ahead of print August 1, 2020;80:105142, Clinical Biomechanics. DOI: 1016/j.clinbiomech.2020.105142.
- Cesar GM, Buster TW, Burnfield JM (2020). Comparison of plantar pressure profile of young adults during training on elliptical devices and overground walking: A pilot study. The Foot. 45: 101716. DOI: 10.1016/j.foot.2020.101716.
- Cesar GM, Buster TW, Burnfield JM (2020). Cardiorespiratory fitness, balance and walking improvements in an adolescent with cerebral palsy (GMFCS II) and autism after motor-assisted elliptical training. European Journal of Physiotherapy, 22(3):124-132. DOI: 10.1080/21679169.2018.1536764.
- Burnfield JM, Buster TW, Pfeifer CM, Irons SL, Cesar GM, Nelson CA (2019). Adapted motor-assisted elliptical for rehabilitation of children with physical disabilities. ASME Journal of Medical Devices, 13(1):011006. DOI: 1115/1.4041588.
- Burnfield JM, Pfeifer CM, Kwapiszeski S, Irons SL, Buster TW, Cesar GM (2019). Impact of ICARE training speed and motor assistance on cardiovascular response. Cardiopulmonary Physical Therapy Journal, 30(3):115-122. DOI: 1097/CPT.0000000000000098.
- Pfeifer CM, Rowen D, Buster TW, Cesar GM, Irons SL, Burnfield JM (2019). Design and validation of a heart rate and speed monitoring device with the ICARE. ASME Journal of Medical Devices. 13(1):015002. DOI: 1115/1.4041337.
- Burnfield JM, Cesar G, Norkin CC (2019). Chapter 7: Examination of Gait. Susan B. O’Sullivan, Thomas J. Schmitz, George D. Fulk (Eds). Physical Rehabilitation, Seventh Edition. F.A. Davis, Philadelphia, PA, pp 228-293.
- Burnfield JM, Cesar GM, Buster TW, Irons SL, Pfeifer CM (2018). Walking and fitness improvements in child with diplegic cerebral palsy following motor-assisted elliptical intervention. Pediatric Physical Therapy, 30(4):E1-E7. DOI: 10.1097/PEP.0000000000000541. PMID: 30277973.
- Burnfield JM, Cesar G, Buster TW, Irons SL, Nelson CA (2017). Kinematic and muscle demand similarities between motor-assisted elliptical training and walking: Implications for pediatric gait rehabilitation. Gait & Posture, 51:194-200. DOI: 10.1016/j.gaitpost.2016.10.018. PMID: 27810692.
- Burnfield JM, Powers CM (2017). Normal and Pathological Gait, Chapter 15. In Placzek JD, Boyce DA (Eds). Orthopaedic Physical Therapy Secrets, Third Edition. Hanley & Belfus. [Bookshelf Online].
- Burnfield JM, Buster TW, Goldman AJ, Corbridge LM, Harper-Hanigan K (2016). Partial body weight support treadmill training speed influences paretic and non-paretic leg muscle activation, stride characteristics, and ratings of perceived exertion during acute stroke rehabilitation. Human Movement Science, 47:16-28. DOI: 10.1016/j.humov.2016.01.012. PMID: 26845732.
- Irons SL, Brusola GA, Buster TW, Burnfield JM (2015). Novel motor-assisted elliptical training intervention improves Six-Minute Walk Test and oxygen cost for an Individual with Progressive Supranuclear Palsy. Cardiopulmonary Physical Therapy Journal, 26(2): 36-41. DOI: 10.1097/CPT.0000000000000007.
- Nelson CA, Stolle CJ, Burnfield JM, Buster TW (2015). Modification of the Intelligently Controlled Assistive Rehabilitation Elliptical (ICARE) system for pediatric therapy. Published online, ASME Journal of Medical Devices, 9(4): 6 pages. DOI: 10.1115/1.4030276.
- Burnfield JM, Irons SL, Buster TW, Taylor AP, Hildner GA, Shu Y (2014). Comparative analysis of speed’s impact on muscle demands during partial body weight support motor-assisted elliptical training. Gait and Posture, 39(1):314-320. DOI: 10.1016/j.gaitpost.2013.07.120. PMID: 23973354.
- Fager SK, Burnfield JM (2014). Patients’ experiences with technology during inpatient rehabilitation: opportunities to support independence and therapeutic engagement. Disability and Rehabilitation: Assistive Technology, 9(2):121-127. DOI: 10.3109/17483107.2013.787124.
- McCrory B, Harlow AH, Burnfield JM (2014). Musculoskeletal risk to physical therapists during overground gait training: A case report. Proceedings of the Human Factors and Ergonomics Society Annual Meeting 10/2014; 58(1):1219-1223. DOI: 10.1177/1541931214581254.
- McCrory B, Burnfield JM, Darragh A, Meza JL, Irons SI, Brusola G, Link AM. (2014). Work injuries among therapists in physical rehabilitation. Proceedings of the Human Factors and Ergonomics Society Annual Meeting 10/2014; 58(1):1072-1076. DOI: 10.1177/1541931214581224.
- Buster TW, Burnfield JM, Taylor AP, Stergiou, N (2013). Lower extremity kinematics during walking and elliptical training in individuals with and without traumatic brain injury. Journal of Neurologic Physical Therapy, 37(4):176-86. DOI: 10.1097/NPT.0000000000000022. PMID: 24189335.
- Burnfield JM, Shu Y, Buster TW, Taylor A, Nelson CA (2011). Impact of elliptical trainer ergonomic modifications on perceptions of safety, comfort, workout and usability for people with physical disabilities and chronic conditions. Physical Therapy, 91(11): 1604-1617. DOI: 10.2522/ptj.20100332. PMCID: PMC3367158.
- Nelson CA, Burnfield JM, Shu Y, Buster TW, Taylor A, Graham A (2011). Modified elliptical machine motor-drive design for assistive gait rehabilitation. ASME Journal of Medical Devices, 5(2) 021001 (May 02, 2011): DOI: 10.1115/1.4003693.
- Burnfield JM, Shu Y, Buster TW, Taylor AP (2010). Similarity of joint kinematics and muscle demands between elliptical training and walking: Implications for practice. Physical Therapy, 90(2):289-305. DOI: 10.2522/ptj.20090033. PMID: 20022994.
- Perry J, Burnfield JM (2010). Gait Analysis, Normal and Pathological Function, 2nd Slack: Thorofare, NJ.
- Kulig K, Burnfield JM (2008). The role of biomechanics in orthopedic and neurological rehabilitation. Acta of Bioengineering and Biomechanics, 10(2):3-14. PMID: 19031992.
- Burnfield JM, Jorde AG, Augustin TR, Augustin TA, Bashford GR (2007). Variations in plantar pressure variables across five cardiovascular exercises. Medicine and Science in Sports and Exercise, 39(11):2012-2020. PMID:
SELECTED ABSTRACTS
- Cesar GM, Buster TW, Patten A, Perlaki BA, Burnfield JM. Reliability and accuracy of commercially-available wrist step-count device for children and adolescents with neurologic-induced gait impairment. 2020 ACRM VIRTUAL Annual Conference.
- Nimmo SM, Catcher BJ, White HJ, Buster TW, Cesar GM, Burnfield JM. Impact of backward motor-assisted elliptical training on upper extremity muscle activation patterns when using reciprocally moving handles. 2020 ACRM VIRTUAL Annual Conference.
- Jacobsen A, Buster TW, Cesar GM, Burnfield JM (2020). Comparison of electromyographic demands on trunk musculature during forward and reverse motor-assisted elliptical training. 2020 ACRM VIRTUAL Annual Conference. October 23, 2020.
- Nalamasu R, Schwery NA, Rasmussen, CM Buster TW, Cesar GM, Burnfield JM (2020). Motor-assistance and resistance during elliptical training alter upper extremity muscle activation patterns when using reciprocally moving handles. American Academy of Physical Medicine and Rehabilitation 2020 Annual Assembly. San Diego, CA. November 12-15, 2020.
- Baker BC, Burnfield JM, Buster TW, Cesar GM, Mestelle Z, Olbrantz CR (2020). Comparison of lower extremity joint kinematics and electromyographic demands during backward walking and reverse motor-assisted elliptical training. American Academy of Physical Medicine and Rehabilitation 2020 Annual Assembly. San Diego, CA. November 12-15, 2020.
- Burnfield JM. ICARE: An integrated approach for addressing gait, fitness, balance and upper extremity rehabilitation goals. Ability KC. Kansas City, MO. November 20, 2019.
- Burnfield JM. ICARE: An integrated approach for addressing gait, cardiorespiratory, balance and upper extremity rehabilitation goals. Rancho Los Amigos National Rehabilitation Center. Downey, CA. November 26, 2018.
- Burnfield JM, Buster TW, Cesar GM, Irons SL, Pfeifer CM. ICARE to improve walking and fitness in adults and children with physical disabilities and chronic conditions (2018). NIDILRR 40th Anniversary Celebration Poster Session. Great Hall of the Hubert H. Humphrey Building, Washington, DC. October 18, 2018.
- Pfeifer CM, Whorley BA, Buster TW, Cesar GM, Burnfield JM (2018). Investigation of center of pressure during gait and motor-assisted elliptical training in adults. Archives of Physical Medicine and Rehabilitation, 99(12):e206. DOI: 10.1016/j.apmr.2018.09.052.
- Huang C-K, Buster TW, Siu K-C, Burnfield JM (2018). Combining virtual reality gaming with motor-assisted elliptical impacts children’s engagement in exercise. Archives of Physical Medicine and Rehabilitation, 99(12):e195. DOI: 10.1016/j.apmr.2018.09.020.
- Burnfield JM. Invited Keynote: Foot and Ankle Rockers: Contributions to Progression, Shock Absorption and Stability during Gait. 2018 Nederlandse Vereniging van Podotherapeuten Conference. Congrescentrum NBC in Nieuwegein, Netherlands. September 21, 2018.
- Burnfield JM. SportsArt ICARE Motor-Assisted Elliptical Training to improve walking, fitness, and wellbeing. International Council on Active Aging (ICAA) Product Webinar. November 6, 2018.
- Burnfield JM. ICARE Clinical Use for Walking, Fitness, Balance and Arm Rehabilitation: An Integrated and Affordable Approach. ExercisABILITIES Physical Therapy and Medical Fitness. Rochester, MN. August 16, 2018.
- Burnfield JM. ICARE: Customizing Use for First Rehabilitation Hospital of Shanghai, China. The First Rehabilitation Hospital of Shanghai, China. April 21, 2018.
- Burnfield JM. Robotic ICARE Technology for Walking, Fitness, Balance and Arm Rehabilitation: An Integrated and Affordable Approach. The 4th China Rehabilitation Forum (CRF2018). Shanghai, China. April 20, 2018.
- Burnfield JM. ICARE: A Practical Rehabilitation Solution to Address Complex Patient Challenges. Osceola Regional Medical Center – HCA. Kissimmee, FL. January 24, 2018.
- Burnfield JM. Improving Walking and Fitness Following Neurologic Injury: Practical Solutions to Complex Challenges. 2018年中美康复医学与研究论坛/ 2018 Sino-US Rehabilitation Medicine and Research Symposium. Shanghai, China. January 15, 2018.
- Cesar GM, Irons SL, Garbin A, Eckels E, Buster TW, Burnfield JM (2017). Child with traumatic brain injury improved gait abilities following intervention with pediatric motor-assisted elliptical training: A case report. Journal of Neurologic Physical Therapy, 41(1):84. DOI: 10.1097/NPT.0000000000000156.
- Irons SL, Buster TW, Karkowski-Schelar E, Johns E, Burnfield JM (2016). Individuals with multiple sclerosis improved walking endurance and decreased fatigue following motor-assisted elliptical training intervention. Archives of Physical Medicine and Rehabilitation, 97(10):e34.
- Burnfield JM, Buster TW, Irons SL, Cesar GM, Nelson CA, Rech NR, Nichols EM (2016). Pediatric walking vs. training on prototype motor-assisted elliptical: Kinematic comparison at self-selected comfortable speed. Archives of Physical Medicine and Rehabilitation, 97(10):e99.
- Burnfield JM, Irons SL, Cesar GM, Buster TW, Khot R, Nelson CA (2016). Pedi-ICARE training improves walking and endurance of child with cerebral palsy. Archives of Physical Medicine and Rehabilitation, 97(12):e19-e20.
- Burnfield JM, Buster TW, Irons SL, Rech N, Cesar GM, Pfeifer CM, Nelson CA (2016). Pediatric Intelligently Controlled Assistive Rehabilitation Elliptical for walking and fitness: Prototype development and biomechanical analysis. RESNA/NCART (Rehabilitation Engineering Society of North America/National Coalition for Assistive and Rehab Technology) 2016 annual convention. Arlington, VA, July 13, 2016.
- Buster TW, Burnfield JM, Irons SL, Nelson CA, Trejo LH, Leutzinger TJ (2016). Pediatric walking vs. training on a prototype motor-assisted elliptical: Kinematic and EMG comparisons at self-selected fast speeds. 2016 Annual Meeting Gait and Clinical Movement Analysis Society. Memphis, TN, May 17-20, 2016.
- Burnfield JM, Irons SL, Buster TW (2016). Individual with progressive supranuclear palsy demonstrates improvements in walking distance and efficiency following a motor-assisted elliptical training intervention. Presented, 9th World Congress for Neurorehabilitation. Philadelphia, PA, May 12, 2016.
- Burnfield JM, Buster TW, Irons SL (2016). Individuals post stroke improved walking endurance and efficiency following motor-assisted elliptical training intervention. Presented, 9th World Congress for Neurorehabilitation. Philadelphia, PA, May 12, 2016.
- Buster TW, Burnfield JM (2016). Movement variability during walking and elliptical exercise for individuals with chronic severe traumatic brain injuries. 9th World Congress for Neurorehabilitation. Philadelphia, PA, May 12, 2016.
- Trejo LH, Buster TW, Stolle CJ, Nelson CA, Burnfield JM. Influence of Rocker and Crank Arm Lengths on Intelligently Controlled Assistive Rehabilitation Elliptical (ICARE) Coupler Trajectories. Biomedical Engineering Career Conference (MBECC) 2014, Detroit, MI. November 7, 2014.
- Burnfield JM. Development and Implementation of the ICARE for Use in Rehabilitation and Fitness. Hospital Corporation of America. Nashville, TN. Presented October 14, 2013.
- Burnfield JM. Desarrollo e implementación del ICARE para uso en rehabilitación y entrenamiento físico. Instituto Nacional De Rehabilitación. Lima, Perú. September 12, 2013.
- Burnfield JM. Desarrollo e implementación del ICARE para uso en rehabilitación y entrenamiento físico. Lima, Peru. September 11, 2013.
- Burnfield JM. ICARE Training to Improve Walking and Cardiovascular Fitness for Individuals Living with Physical Disabilities and Chronic Conditions. Quality Living Incorporated. Omaha, NE. Presented April 10, 2013.
- Burnfield JM. ICARE Training to Improve Walking and Cardiovascular Fitness for Individuals Living with Physical Disabilities and Chronic Conditions. Marionjoy Rehabilitation Hospital. Wheaton, IL. Presented April 24-25, 2012.
- Burnfield JM. ICARE Training to Improve Walking and Cardiovascular Fitness for Individuals Living with Physical Disabilities and Chronic Conditions. Hospital for Special Care. New Britain, CT. Presented April 2-3, 2012.
- Yeseta MC, Taylor AP, Buster TW, Shu Y, Burnfield JM (2012). Exercise endurance and functional mobility improve for individuals with physical disabilities after training on a motorized elliptical. Online proceedings, Rehabilitation Engineering and Assistive Technology Society of North America’s 2012 Annual Conference.
- Nelson, CA. Burnfield JM (2012). Improved elliptical trainer biomechanics using a modified Cardan gear. Proceedings of the ASME 2012 International Design Engineering Technical Conference & Computers and Information in Engineering Conference [Conference Paper #: DETC2012-70439]. Chicago, IL.
- Burnfield JM, Yeseta M, Buster TW, Taylor AP, Shu Y (2012). Individuals with physical limitations can benefit from training on a motorized elliptical for community-based exercise. Medicine and Science in Sports and Exercise, 44(5 Supplement), pg. 524.
- Taylor AP, Lowndes BR, Buster TW, Shu Y, Burnfield JM (2012). Speed’s impact on pedar pressures at varying levels of body weight supported ICARE training. Proceedings, Gait and Clinical Movement Analysis Society 2012 Annual Meeting, pg 139-140.
- Shu Y, Taylor AP, Buster TW, Burnfield JM (2012). Clinicians’ motion and muscle activation patterns during body weight support treadmill training. Proceedings, Gait and Clinical Movement Analysis Society 2012 Annual Meeting, pgs. 230-231.
- Buster TW, Goulet C, Shafer D, Burnfield JM (2012). Comparison of kinematic demands of walking and elliptical training between individuals with and without mild to moderate multiple sclerosis. Proceedings, Gait and Clinical Movement Analysis Society 2012 Annual Meeting, pgs. 232-233.
- Burnfield JM. ICARE Training to Improve Walking and Cardiovascular Fitness for Individuals Living with Physical Disabilities and Chronic Conditions. JFK Johnson Rehabilitation Institute. Edison, NJ. Presented March 26-27, 2012.
- Burnfield JM, Hildner GA, Buster TW, Taylor AP, Shu Y (2011). Speed’s impact on muscle demands during partial body weight supported training on a motorized elliptical. Archives of Physical Medicine and Rehabilitation, 92(10): 1700.
- Burnfield JM, Taylor AP, Buster TW, Shu Y, Goldman AJ, Nelson CA (2011). Use of Intelligently Controlled Assistive Rehabilitation Elliptical trainer to improve walking and fitness during acute stroke rehabilitation. Stroke, 42(3), pg. e326.
Selected Professional Presentations
- Burnfield JM, Goulet C, Buster TW, Cassel AJ, Mills J, Seow CM (2011). Comparison of velocity, muscle demands and perceived exertion during elliptical training and treadmill walking in individuals with and without multiple sclerosis.Annual Combined Sections Meeting of the American Physical Therapy Association.
- Burnfield JM, Shu Y, Buster TW, Taylor AP, Merriman L, Nelson CA (2010). Comparison of lower extremity electromyographic (EMG) demands during ICARE training and walking. Online Proceedings, American Society of Biomechanics 34th Annual Meeting.
- Buster TW, Taylor AP, Frazier M, Burnfield JM (2010). Kinematic analysis of five cardiovascular exercises. Online Proceedings, American Society of Biomechanics 34th Annual Meeting.
- Burnfield JM, Buster TW, Taylor A, Keenan S, Shu Y, Nelson CA (2010). Intelligently Controlled Assistive Rehabilitation Elliptical (ICARE) Training: An Analysis of Lower Extremity Electromyographic (EMG) Demands with Varying Levels of Motor Assistance. Online Proceedings, Rehabilitation Engineering and Assistive Technology Society of North America’s 2010 Annual Conference.
- Taylor AP, Buster TW, Barber BR, Burnfield JM (2009). Comparison of Forefoot and Heel Pressures across Fast Walking and Four Elliptical Trainer Conditions. Supplement to Medicine and Science in Sports and Exercise, Volume 41(5), pg. S242.
- Corbridge LM, Goldman AJ, Shu Y, Buster TW, Burnfield JM (2009). Clinician’s Muscle Effort during Partial Body Weight Support Treadmill Training: Is it Hard Work?American Physical Therapy Association’s 2009 Annual Conference and Exposition.
- Buster TW, Goldman AJ, Corbridge LM, Shu Y, Burnfield JM (2009). Partial Body Weight Support Treadmill Training: Clinician’s Upper Extremity Muscle Activation During Facilitation of Hemiparetic Limb Movement. Proceedings, Gait and Clinical Movement Analysis Society 14th Annual Meeting, pgs 258-259.
HEAR FROM PATIENTS
BRANDON & TIFFANY
Parents of TBI Patient
SHAUNA
Stroke Patient
ALEX
Incomplete Spinal Cord Injury Patient
GAVIN
Stroke Patient
Robert J. McIver, PT, DPT, NCS
Director of Clinical Technology and Wellness
Brooks Neuro-Recovery Center Jacksonville, FL
We have had the ICARE at Brooks Rehabilitation for over 2 years now. It is one of our most highly utilised pieces of equipment. We use the ICARE to treat patients with any gait or balance impairments regardless of diagnosis; Orthopaedic, Neurologic, Geriatric, Bariatric, and Paediatric. The patients and staff love using the ICARE due to the versatility it provides as well as the ease of set up. The adjustability of speed and stride length ensure that training is customised to each patient and their specific needs. We have patients who come in just to use the ICARE in our independent programme to maintain their health and quality of life.
The staff that uses it enjoy that we can provide longer sessions of stepping with less assist from other staff and less need to muscle through a locomotor session on the treadmill. It also provides a way to increase stepping in a safe environment that we can work on functional tasks such as reaching and trunk rotations while the lower legs are moving to increase dynamic balance. Mostly, staff and patients like the fact that regardless of the level of function of the patient the ICARE provides the means to deliver a cardiovascular workout that no other machine can deliver.
We had a patient with a lumbar plexus palsy that was not able to generate a static EMG in his doctor’s office, but when using the ICARE at a higher speed was able to generate a dynamic EMG. After months of rehab using the ICARE the patient was able to return to running and playing with his children with no assistive devices. His prognosis prior to this discovery and intervention would be all standing and walking tasks would need a locking knee brace.
Overall, the ICARE is a very affordable piece of rehabilitation technology that allows any clinician to deliver a highly intense intervention that can be geared toward any patient population.
Liza Reidel
Executive Director
NextStep Orlando (Previously Project Walk Orlando)
Project Walk Orlando’s mission is to provide those living with spinal cord injuries the opportunity to achieve their greatest recovery potential and an increased quality of life. Our mission is fulfilled by providing specialised one-on-one, cutting-edge, aggressive and comprehensive exercise-based programmes. The ICARE system has played an integral role in helping our clients and staff achieve this mission.
The ICARE system is utilised on a daily basis during clients exercise programmes to provide an intensive cardiovascular and gait training workout. From a client and staff perspective, the ICARE has been a successful addition to our facility, allowing for an efficient setup and for the trainer to ensure the client is in a comfortable and safe position. Clients are able to achieve thousands of steps on the ICARE system which supports the repetitive movement science of SCI training. In addition to this, clients are able to make use of the feedback function where if they move the elliptical faster than the motor speed the machine lets them know. This function always increases their effort and motivation during the workout.
Various factors weighed into the decision to fundraise and purchase the ICARE System for PWO. These include the systems ability to improve our clients’ fitness, circulation and function in a manner which is less labour intensive on trainers. The ICARE can provide our clients with 1000’s of steps that would typically require multiple trainers, assistants and a lot of time.